Endeavour
Beyond Borders
ICDDR,B's expertise in cholera management is having a profound impact in other parts of the world
Shudeepto Ariquzzaman
 |
Travelling through the rough terrains of Zimbabwe. Photo: ICDDR,B |
In 1994, a brutal conflict lasting approximately 100 days resulted in the deaths of nearly 800,000 people in the African nation of Rwanda. As a result of the conflict, nearly a million refugees escaped to Goma, eastern Congo (then known as Zaire). They were concentrated in several regions across the Goma region. The refugee camps lacking water supply and sanitation were fertile breeding grounds for cholera. Within weeks the epidemic took root in the camp leading to approximately 12,000 deaths. according to the estimates of United Nations High Commission for Refugees.
Generally, Bangladesh, an impoverished country with so many disasters to her own name, seems an unlikely place to look for assistance when disasters occur in another part of the globe. Yet that is what the US State Department decided to do in wake of the cholera crisis in Goma. The call of assistance was made to International Centre for Diarrhoeal Disease Research, Bangladesh (ICDDR,B), an institution that has made remarkable breakthroughs in combating cholera.
However, once the ICDDR,B medical team arrived in Goma, they faced numerous difficulties and it seemed almost impossible that they could be operational in such a short period. Dr AK Siddique, the team leader and Consultant Epidemiologist at ICDDR,B describes the situation: “for nearly six hours we were stranded in the small tent with no apparent way for our team to contribute to the situation. I had no logistical support, no hope of any assistance, or enough money.”
“We did not have IV fluid or ORS (oral rehydration solution). Nor did we have any drugs. I went to the UNICEF office,” says Dr Siddique.
As it turned out, there was someone from Eastern Mediterranean UNICEF office, who had trained at ICDDR, B three months before. He was quite relieved to see Dr Siddique and the ICDDR, B team. The UNICEF officials had a positive view of ICDDR,B and were willing to provide the necessary supplies. But they pointed out to Dr Siddique that there was still another barrier – permission needed to be forthcoming from the local Zairan Health Officer, and he knew no English, only French and Swahili.
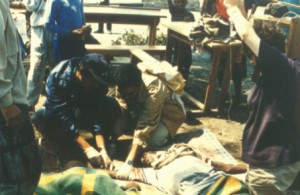 |
The contributions of the ICDDR, B team in Goma showed that even in a disaster setting, the odds of death from cholera could be minimised. Photo: ICDDR,B |
Fortunately Dr Siddique was well versed in Swahili. He told the health officer, that cholera would not necessarily be confined only to the refugees but might spread among the local population if immediate steps were not taken. In that case, Dr Siddique told the health officer that he would be the one blamed by everyone. The ploy worked. “Within an hour, we set up a makeshift treatment centre. I had UNICEF biscuits, water cans, medicines, ORS, IV fluid- better supplies than anyone else.”
ICCDR, B assistance brought quick results. In Katindo treatment centre, the effects were felt almost immediately. The contributions of the ICDDR,B team showed that even in a disaster setting, the odds of death from cholera could be minimised.
From July 22- 27, 1994, when the Rwandan medical staff was acting alone, the case-fatality ratio was 14.5 percent, 115 deaths out of 790 cases. The ICDDR, B took over from July 28. In the next two days, from July 28- July 29, the case-fatality ratio reduced to 3 percent, with 12 deaths reported from 399 cases. The ICDDR,B assisted only by the Rwandan staff operated from July 30- August 3. The case fatality ratio reduced to 0.6 percent, with three fatalities from 536 cases.
Since then, the ICDDR,B's global response teams have been called upon to assist cholera epidemics in different parts of the world the most notable being recent missions in Pakistan and Zimbabwe. Most recently, on November 13, 2010 a team of experts in clinical management and epidemic control from ICDDR,B set off for Haiti to assist the international community in managing the country's cholera epidemic.
The team to Haiti consisted of Dr R N Mazumder, Dr Pradip K Bardhan, Dr Azharul Islam Khan, Dr Zahid Hayat Mahmud, Dr KATM Ehsanul Huq, Dr Sharifuzzaman, Dr Chandra Shakhar and Nursing Officers Momtaz Begum and Catherine Costa. They provided technical assistance to three organisations- Project Hope, Centres for Disease Control and Preventio Atalanta, USA and the World Health Organisation.
This is the first time in a century that cholera has struck the impoverished Caribbean nation, still suffering from the aftereffects of the massive earthquake of 7.0 magnitude which has basically destroyed the infrastructure of the nation. Death tolls have surpassed 2,000 and still rising.
“They are having a very difficult time,” says Dr Pradip K Bardhan, a clinician who has along with the other team members just returned from Haiti. “ The earthquake has left the country devastated. Approximately ten per cent of the population is internally displaced, that is excluding the substantial populace who already resided in the slums.”
Dr Bardhan reflecting on his previous experience in Zimbabwe says, “Zimbabwe was once known as the bread basket of Africa. Although the infrastructure is not as good as before, still there is something. In Haiti this is not the case.” He says that Haiti never had the proper infrastructure and the earthquake has destroyed whatever little there was.
The health professionals and hospital staff of Haiti had reacted to the cholera crisis with extreme panic and possessed little knowledge on how to combat this deadly disease. “We have trained hundreds of medical staff and there has been results,” says Dr Bardhan. “The number of patients have not of course lessened, that is impossible for us, but the fatality rate has decreased.”
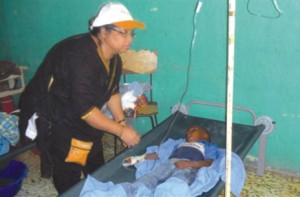 |
One of the two patients who were left for dead in Haiti. Photo: ICDDR,B |
He says that in a country which has not experienced cholera in a century, the level of awareness is understandably low, not only among the general populace but among doctors and health professionals as well. This is where ICDDR,B's expertise has made the most profound impact. “We have the practice, the experience needed for combating cholera,” he says. “We can identify the lapses, work on long term solutions and conduct training of trainers.” Incidentally the cholera bacteria first originated in the lower Ganges delta (modern day Bangladesh) and the country has substantial experience in dealing with the epidemic that has once wiped out village after village in this region of Bengal.
Dr Bardhan says that training all health workers who are required to combat the cholera crisis in Haiti is an unfeasible task, let alone treating all the cholera patients. “So we concentrate on training of trainers. We train medical staff who subsequently disperse their knowledge to other staff.”
Other members of the team back up his statement regarding the lack of awareness that acts as the main deterrent in the war against cholera. They say that even the senior most doctors of the country know nothing about cholera and are in total panic. Dr R N Mazumder, clinician and the team leader describes the dire conditions of Haiti that makes the place fertile breeding grounds for cholera. “Sixty percent of the population has no access to safe drinking water. The earthquake has totally destroyed the sewerage system and the people are living in overcrowded and cramped conditions,” he says. “Then there is the management issue – they simply did not understand the treatment procedures at all.”
“Cholera is easy to diagnose, easy to treat and nothing to worry, these are the three things we tried to instill in their minds,” says Dr Mazumdar. Although cholera is both preventable and treatable, it still claims so many lives because of the lack of knowledge concerning the disease.
According to Dr Md Sirajul Islam, a microbiologist, Haiti might face food insecurity in the future, as farmers are afraid to go to the fields to gather their harvest for fear that they might contract cholera. “Once I had tested the water and assured them there was no cholera in one of the rivers where the disease once originated, they gathered the courage to go to the fields,” he says. Of course, the testing was irrelevant; Dr Islam knew very well that the water would not be contaminated with cholera for so long. But in Haiti everybody seems to be in a panic. “Haiti has become a society where there are no more handshakes,” he says. Apparently people suppose cholera, which is in fact a water-borne disease, can be transmitted through physical contact.
“Health workers have vague and misleading concepts,” says Dr Bardhan, “One health worker asked me if the smell from the cholera stool might spread cholera.” He emphasises that if trained health workers have no consciousness regarding the disease, one can wonder the lack of consciousness that exists among the populace.
“In our training sessions, primary school students to college students have come to gain knowledge,” says Dr Zahid Hayat Mahmud, an assistant scientist reaffirms that after every training session, the audience seemed more reassured.
Momtaz Begum, one of the two nurses who had accompanied the team also recalls her surprise when she saw health workers dressed with gumboots and flap jackets. “Once they saw that we were dressed normally, they were more relaxed,” she says. “We had to teach them how to handle the cases properly and not to react with panic. An HIV patient told us that with his disease, he can last 20 years but if he contracts cholera, he is going to die within hours. But we told the audience, that these are misleading concepts.” This is the first time nurses had accompanied the global team, at substantial risk to their own safety.
She recalls with disappointment that as elections take place, posters of different candidates are displayed across the country. “Instead, the government could have made posters carrying messages that spread awareness about cholera,” she says.
The medical team recounts what they describe as their best experience in Haiti. “In one of the camps, we saw two severely ill patients. The local doctors thought they had no hope left and they were simply left to die,” says Momtaz Begum. “After administering four litres of IV fluid, they had completely recovered. It was the best experience of the whole mission, that we could save them.” The incident only demonstrates the efficiency of the Bangladeshis in comparison to their counterparts. Also it is evidence that when it comes to cholera, knowledge carries power in saving lives.
In spite of the dreadful conditions prevailing in Haiti, the medical team recounts with pleasure the friendship extended by the people of Haiti towards them. This is in stark contrast to the feelings many international aid workers have towards the disaster struck populace of the country. “They accepted us as friends,” says Begum. “In a church, a priest prayed for us and praised us for coming from another part of the world to help them.”
Dr Bardhan also recounts with pleasure their experiences abroad. “ It feels good,” he says, “we feel proud that we are not only representing ICDDR,B but the entire nation of Bangladesh.”
Copyright
(R) thedailystar.net 2010 |
| |
